The Myth of the Negative Mammogram
January 9th, 2012It is a scenario familiar to all breast imaging practices.
A patient feels a lump in her breast and calls her doctor. The doctor examines her, agrees that a lump is present, and refers the patient to a breast imaging facility for a diagnostic mammogram and breast ultrasound (also known as a sonogram). At her mammogram appointment, a little sticker is placed on the lump felt by the patient, and mammogram images are taken. Something may or may not be seen on the mammogram at the site of the lump. A breast sonogram is performed, and a suspicious mass is seen, clear as day. …
Read MoreDiagnosed with Breast Cancer as a New Mother, Sharon Shares her Story
December 6th, 2011In 2003, my mom friend Sharon was relishing her role as a new mother in her early 40’s. She’d given birth to her daughter in 2001, and was now busy chasing after an adorable toddler, navigating naptimes, bottles and diapers, while working in the banking industry in Manhattan. Her husband and their brother-in-law had renovated and opened a beautiful new restaurant, and life was very exciting.
The Symptom Leading to Diagnosis
Sharon had gone for yearly mammograms since turning 40, and the test had always been reported as normal. She had no family history of breast…
Read MoreResponse to NY Times article: Mammogram’s Role as Savior Is Tested
November 2nd, 2011Tara Parker-Pope’s recent article in the New York Times Science Section discounts the role of mammography as an essential tool in the quest to save women from premature death due to breast cancer. She reports on the conclusion drawn by researchers Welch and Frankel from Dartmouth, who published a statistical analysis using epidemiologic data and computer software in this article in Archives of Internal Medicine this month. Their conclusion: “Most women with screen-detected breast cancer have not had their life saved by screening. They are instead either…
Read MoreBreast Density Advocates on Good Morning America
October 13th, 2011Nancy Cappello, PhD and JoAnn Pushkin were interviewed on Good Morning America last week, talking about their experiences as women doing “everything right”: mammograms every year, healthy lifestyle, annual checkups. Yet even though they were good, compliant patients, they both were diagnosed with advanced breast cancers. How did this happen? Well, they were never informed that they have dense breast tissue, which confers an increased risk for breast cancer, AND makes a mammogram so hard to read that up to half of cancers won’t be seen.
Since they were given “normal”…
Read MoreWhen Should I Have My First Mammogram?
October 4th, 2011General Guidelines
For most women, age 40 should be when you start having yearly mammograms in order to minimize your likelihood of developing advanced breast cancer (“Government Mammography Task Force vs. You”). Some doctors send their patients for a baseline mammogram at age 35, and I wouldn’t argue with that.
Family History
If you have a strong family history of breast cancer (mother or sister), start having your mammogram 10 years younger than the age that relative was diagnosed, OR at age 40, whichever is younger. For example, if your sister had breast cancer…
Read MoreCase Example: Self-Examination Saved Her
September 16th, 2011As follow-up to my last post regarding breast self-examination, I offer a real case example:
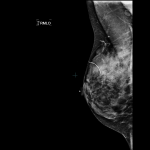
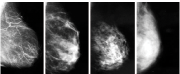
A 39-year-old mom with no family history of breast cancer felt a lump in her right breast when she was doing a self-examination. Her mammogram pictures show dense breast tissue. A triangular-shaped sticker (you can see the triangle on the RMLO and RCC films) has been put on the lump. At that site on the mammogram, there is an irregular mass best seen on the magnified view RMML (yellow arrow) that demonstrates “spiculated margins”- a radiology term for badness. The mass…
Read More